In September 2015, the Centers for Disease Control and Prevention (CDC) revised their estimates, indicating that more than 329,000 new cases of Lyme disease were contracted each year in the US — an increase of up to 10 times of what was previously believed. The report also stated that 95% of confirmed Lyme disease cases were reported from only 14 states. The main geographic territory ranges from Maine to Virginia along the East Coast and the upper Midwest states of Wisconsin and Minnesota. This is exactly why diagnosing Lyme disease has become more important than ever before.
With these startling numbers and more and more cases of Lyme disease beginning to take hold on patients, nurses are struggling to properly diagnose the ailment. With symptoms that can vary and mimic those of other illnesses, it can lead many nurses playing detective with very little to go on. Diagnosing Lyme disease can be difficult, but here are a few things that nurses can look out for.
Diagnosing Lyme Disease
The Struggle
There are many factors that come into play when you’re beginning your attempt at diagnosing Lyme disease. One of the biggest issues that many health care professionals will face is having a patient that already has one or multiple pre-existing conditions. In many cases, these symptoms can often be jumbled together, and it can be nearly impossible to distinguish a symptom or side effect from previous conditions to that of a possible case of Lyme disease. Unfortunately, many nurses simply won’t see a patient come into the office until the disease has taken its toll. Many will attribute muscle fatigue, headaches, and overall exhaustion to old age or a stressful life, when, in fact, it could be Lyme disease taking a toll on the patient’s body. This is yet another reason that nurses must play detective and try to find the best possible diagnosis that they can come up with.
Common Symptoms
While there are a variety of symptoms that Lyme disease can cause, it’s more important to look and see if your patients have multiple signs that point towards Lyme disease. These symptoms include:
- Fatigue
- Headache
- Joint pain
- Rash
- Muscle pain
- Fever
- Sweats
- Sleep Issues
- Chills
- Confusion
- Neuropathy
While many of these seem like your typical flu-like symptoms, it’s important that you do some detective work as a nurse. If your patient is reporting a few of these symptoms, make sure you look into some Lyme disease tests so you can try to make a definitive prognosis. It’s also a good idea to look into a patient’s history. For example, find out if they spend a lot of time in the woods or other places that ticks dwell in, and ask if they’ve noticed any “bulls-eye” marks that could indicate an infected tick bite.
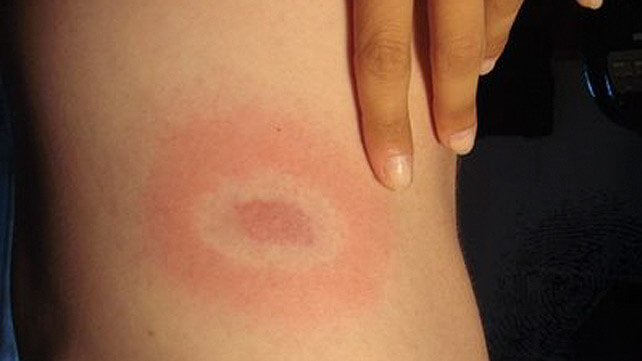
A bullseye rash is one of the most common indicators of Lyme disease.
Testing For Lyme Disease
When diagnosing Lyme disease, there are a few different tests that you should consider to ensure that you’re giving the proper diagnosis to your patients. Here are a few tests that you might want to consider when diagnosing Lyme disease:
Enzyme-link immunosorbent assay test (ELISA) – The test used most often to detect Lyme disease, ELISA, detects antibodies to B. Burgdorferi. However, because it can sometimes provide false-positive results, it can often lead to false-positives, especially if the disease is in its early stages.
Western Blot Test – Similar to the ELISA, this test is often used after a positive ELISA test is confirmed. This one-two punch will essentially confirm that your patient has contracted Lyme disease.
Treatment
The final step in diagnosing Lyme disease is to discover the proper treatment for the disease. In most cases, antibiotics will be the main treatment option for your patients. These oral or intravenous antibiotics will help your patient’s body fight the disease so they can live a happy and healthy life. A 14- to 21-day course of antibiotics is usually recommended, but some studies suggest that courses lasting 10 to 14 days are equally effective. However, some patients may continue to show signs even after treatment, so make sure to perform routine checkups with them so you can help combat some of the symptoms when possible.
